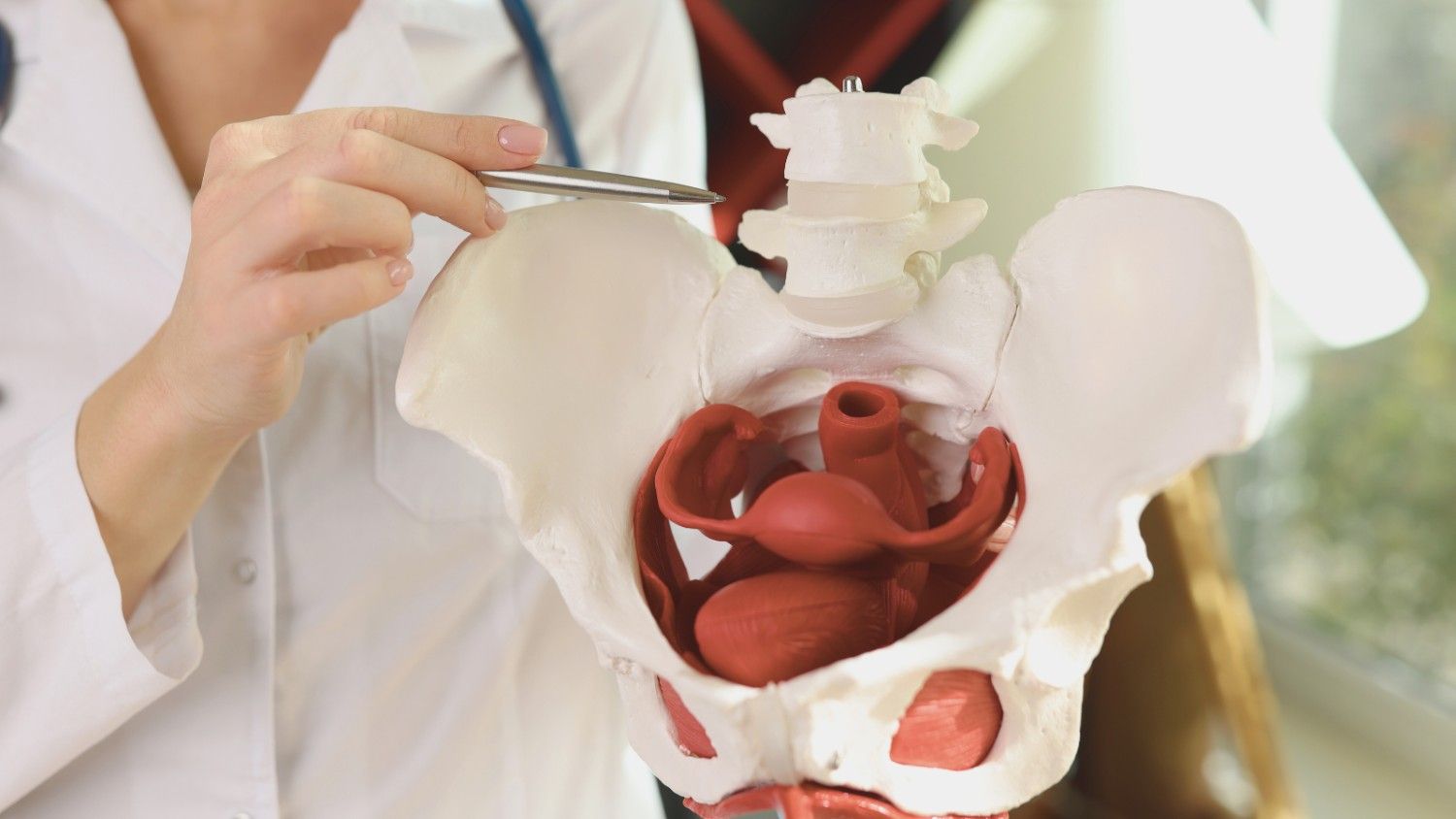
Your pelvic floor during pregnancy supports the growing weight of your baby, placenta and amniotic fluid for 40 weeks. That sustained pressure, combined with hormonal changes that soften the muscles and ligaments in the pelvis, puts these muscles under more strain than at any other point in your life. Stress urinary incontinence affects roughly 54 percent of pregnant women, and up to 1 in 3 women report pelvic floor symptoms after delivery.
The good news is that most pregnancy pelvic floor problems are preventable or manageable with targeted exercises and daily habits started early. Your OBGYN can assess your pelvic floor health as part of your prenatal care and connect you with a pelvic floor physical therapist if you need individualized guidance.
What Does Your Pelvic Floor Do During Pregnancy?
The pelvic floor is a sling of muscles and connective tissue stretching from the pubic bone to the tailbone. These muscles support the bladder, uterus, vagina and rectum and work with the abdominal muscles, diaphragm and glutes as part of your core. During pregnancy, the pelvic floor bears the increasing weight of the baby and the expanding uterus while also helping control bladder and bowel function.
The hormone relaxin rises during pregnancy and softens connective tissue and ligaments throughout the pelvis. This loosening is necessary to prepare the body for delivery, but it also reduces the structural support the pelvic floor provides. Research shows that perineal muscle strength decreases from around week 20 of pregnancy through 6 weeks postpartum. Understanding how your pelvic floor connects to your overall well-being helps explain why proactive strengthening during pregnancy matters so much.
What Pelvic Floor Problems Are Most Common During Pregnancy?
Pregnancy pelvic floor problems develop gradually as the demands on these muscles increase trimester by trimester. Recognizing symptoms early gives you the best chance of managing them before they progress.
Stress Urinary Incontinence
Stress Urinary Incontinence Stress urinary incontinence is the most common pelvic floor during pregnancy. It involves leaking urine when coughing, sneezing, laughing, lifting or exercising. The weight of the growing uterus presses down on the bladder while weakened muscle support makes it harder to maintain a tight seal around the urethra. Roughly 54 percent of pregnant women experience some degree of stress incontinence, with symptoms often appearing in the second trimester and increasing as the baby grows.
Leaking during pregnancy is common, but it is not something you should accept as unavoidable. Targeted pelvic floor training can reduce or prevent it. Women who begin Kegel exercises early in pregnancy are significantly less likely to develop incontinence in the third trimester and during the first three months after delivery. If leaking is already affecting your daily activities or exercise routine, bring it up at your next prenatal visit so your OBGYN can assess the severity and recommend a plan.
Pelvic Pressure and Pelvic Organ Prolapse
Pelvic Pressure and Pelvic Organ Prolapse Pelvic organ prolapse occurs when the muscles and connective tissue can no longer hold the bladder, uterus or rectum in their normal position. Symptoms include a feeling of heaviness, fullness or a bulging sensation in the vaginal area that often worsens after standing for long periods or at the end of the day. Pregnancy and vaginal childbirth are the primary causes of pelvic organ prolapse according to ACOG, and women in the United States have a 13 percent lifetime risk of needing surgery for prolapse or stress urinary incontinence.
Some women notice early signs during pregnancy, while others develop symptoms weeks or months after delivery. Prolapse symptoms can range from mild pressure that comes and goes to a persistent bulge that affects daily comfort and intimacy. Learning to recognize the signs of pelvic organ prolapse early allows your OBGYN to recommend the right intervention before the condition worsens.
Pelvic Pain and Lower Back Pain
Pelvic Pain and Lower Back Pain Pelvic girdle pain affects many pregnant women as the hormone relaxin loosens the joints and ligaments in the pelvis. The shift in your center of gravity as the baby grows changes your posture and places additional strain on the lower back and pelvic muscles. Pain may show up as a deep ache across the front of the pelvis, discomfort in the sacroiliac joints at the back of the pelvis or sharp pain during movements like rolling over in bed, climbing stairs or getting out of a car.
A weak or uncoordinated pelvic floor contributes to core instability, which can make third trimester back pain worse. Strengthening the pelvic floor alongside the deep core muscles helps distribute the load more evenly and reduce pain. If pelvic or lower back pain limits your ability to walk, sleep or carry out daily tasks, your OBGYN can refer you to a pelvic floor physical therapist for a targeted treatment plan.
How to Strengthen Your Pelvic Floor During Pregnancy
Starting pelvic floor exercises pregnancy routines in the first trimester gives these muscles the best foundation for the demands ahead. The earlier you begin, the stronger your pelvic floor will be by the time the baby’s weight peaks in the third trimester.
Kegel Exercises (Pelvic Floor Muscle Training)
Kegel exercises target the muscles you would use to stop the flow of urine or hold in gas. Use that mental cue to identify the correct muscles, but do not practice Kegels while actually urinating because interrupting the stream regularly can affect bladder function.
Effective Kegel training includes two types of contractions:
- Quick flicks: Rapidly contract and release the pelvic floor muscles 10 times in a row. These train the fast-twitch muscle fibers that respond to sudden pressure like a cough or sneeze.
- Sustained holds: Contract the pelvic floor, hold for 5 to 10 seconds, then fully relax for the same amount of time. Repeat 10 times. These train the slow-twitch fibers responsible for ongoing support throughout the day.
Aim for 3 sets of each type daily. You can perform Kegels lying down (easiest), sitting or standing (most challenging). Research shows that Kegel exercises during pregnancy significantly reduce the development of urinary incontinence from 6 weeks to 3 months after delivery.
The Knack Technique
The Knack is a simple habit that protects your pelvic floor in real-time situations. Before you cough, sneeze, laugh or lift something, consciously contract your pelvic floor muscles first. This pre-contraction braces the muscles against the sudden spike in abdominal pressure that causes leaking. Practicing the Knack trains your pelvic floor to respond automatically over time, turning a deliberate effort into a reflex.
Breathing and Core Coordination
The pelvic floor and diaphragm move together during breathing. When you inhale, both lower. When you exhale, both rise. Coordinating your breath with pelvic floor engagement improves the effectiveness of every contraction.
Practice exhaling on effort: breathe out as you lift, stand up from a chair or exert force. This pattern engages the pelvic floor at the moment it needs support most. Deep squats with conscious pelvic floor engagement, prenatal yoga and swimming are all activities that reinforce this coordination. ACOG recommends 150 minutes of moderate aerobic activity per week during pregnancy, along with strength training at least twice weekly. Including pelvic floor work within your pregnancy exercise routine gives these muscles the same attention as any other muscle group.
Daily Habits That Protect Your Pelvic Floor

Exercises build strength, but daily habits determine how much pressure your pelvic floor absorbs between workouts. Small changes throughout your day add up over 40 weeks.
- Prevent chronic constipation by eating fiber-rich foods and drinking plenty of water. Straining during bowel movements puts repeated downward pressure on the pelvic floor.
- Practice proper lifting technique by engaging your pelvic floor and exhaling before you lift. Keep loads close to your body and bend at the knees rather than the waist.
- Avoid prolonged standing without breaks. Shift your weight, walk around or sit down periodically to reduce sustained pelvic pressure.
- Maintain good seated posture with your back supported and both feet on the floor.
- Manage your weight gain within ACOG-recommended ranges to avoid excess pressure on the pelvic floor.
- Adjust your sleep position as your pregnancy progresses to reduce pelvic and lower back strain overnight.
How Does Delivery Affect the Pelvic Floor?
Vaginal Delivery
The pelvic floor muscles stretch significantly during vaginal birth to allow the baby to pass through the birth canal. Perineal tearing can occur in varying degrees, from minor surface tears (grade 1) to deeper tears involving the anal sphincter (grades 3 and 4). Research indicates that pelvic floor muscle training during pregnancy may reduce tearing risk and lower episiotomy rates. Women who maintain a strong, flexible pelvic floor heading into delivery tend to push more effectively and recover faster afterward.
Cesarean Delivery
Cesarean delivery involves less direct stretch and trauma to the pelvic floor muscles during the birth itself. Pregnancy alone weakens the pelvic floor over nine months regardless of how the baby is delivered. The weight of the uterus, the effects of relaxation and the postural changes of pregnancy all affect these muscles independent of the delivery method. Women who deliver by cesarean still benefit from prenatal and postpartum pelvic floor training to restore strength and prevent long-term dysfunction.
When to See a Pelvic Floor Physical Therapist
Talk to your OBGYN about a referral to a pelvic floor physical therapist if you experience any of these during pregnancy or postpartum:
- Leaking urine regularly during daily activities or exercise
- Pelvic heaviness or pressure that worsens as the day goes on
- Persistent pelvic pain that affects daily routines or intimacy
- Unsure if you are performing Kegels correctly (many women engage the wrong muscles without realizing it)
- Incontinence or prolapse symptoms continuing beyond 12 weeks postpartum
Postpartum pelvic floor muscle training reduces urinary incontinence odds by 37 percent and pelvic organ prolapse odds by 56 percent based on a systematic review of over 21,000 participants. Starting pelvic floor work during pregnancy and continuing it after delivery gives you the strongest foundation for long-term pelvic health.
Pelvic Floor Care in Alpharetta, Atlanta, Canton and Cumming
The OBGYNs at Roswell Ob/Gyn, LLC offer a dedicated pelvic floor rehabilitation program that includes therapy for pelvic organ prolapse, urinary incontinence and postpartum recovery. The team at Roswell Ob/Gyn, LLC can evaluate your pelvic floor health during pregnancy and connect you with the right care plan for your needs.
Roswell Ob/Gyn, LLC has offices in Alpharetta, Atlanta, Canton and Cumming. Schedule your appointment today to start protecting your pelvic floor during pregnancy.

